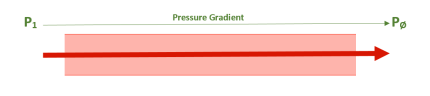
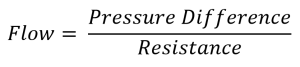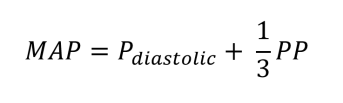Blood flow always travels down a pressure gradient of high to low.
The value for pressure difference is gained with:

And the basic calculation for discerning resistance:
Blood flow is given by:
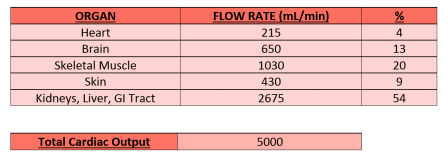
The distribution of systemic blood flow at rest
Distribution is determined by
- Blood pressure
- Vascular resistance
Vessel diameter largely determines blood pressure. There is always some level of resistance within blood vessels, but in smaller vessels, resistance is increased. The diagram below shows the relationship between vessel diameter and blood pressure by illustrating how velocity is affected by surface area.
 Slowed flow, coupled with the large surface area allow for efficient O2 transfer in organs.
Slowed flow, coupled with the large surface area allow for efficient O2 transfer in organs.
Systole
- The period of contraction of the ventricles
- Occurs between the first and second heart sounds
- Causes ejection of blood into the aorta and the pulmonary trunk
- Arterial blood pressure reaches its peak
Diastole
- The period of relaxation of the cardiac muscle
- Followed by systole in the cardiac cycle
- When atria are in systole, blood pressure is at its minimum
- Arterial pressure is troughed
Pulse pressure (PP) can be calculated by subtracting diastolic pressure from systolic pressure.
During the cardiac cycle, pressure is illustrated thusly:
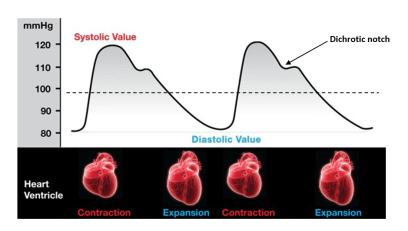
The closure of the aortic valve gives the dichrotic notch.
The dashed line represents mean arterial pressure (MAP) and is given by
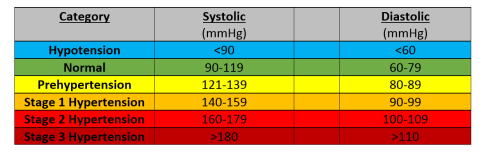
Clinical blood pressure
Blood pressure measurements are categorised according to these boundaries:
We will see, however, that there are many factors that can influence blood pressure measurements and perhaps give false indications.
Clinical measurement
There are many things to consider when measuring blood pressure. The British Hypertension Society offers guidelines on measurement with both manual and automatic devices, and to gain a reading that is as accurate as possible, it is important to:
- Ensure the patient is relaxed, seated and silent for a minimum of five minutes before measurement
- Blood pressure increases with heart rate and cardiac output, so it is important to ensure that the patient’s heart rate is as close to normal as it can be.
- Have the patient’s feet supported and uncrossed, with their back supported.
- Make sure the arm is supported at the level of the heart, with no constriction
- For patient comfort, it is acceptable to provide a pillow or blanket to support the patient’s arm. This will also promote relaxation in the patient.
- The cuff is placed neatly on the arm, appropriately over the brachial artery.
- Appropriate cuff size is often indicated on the interior surface of the cuff itself. Boundaries are given so as to inform of the need for a cuff of increased of decreased size and to allow the practitioner to obtain an accurate blood pressure measurement, regardless of patient dimensions.
- The size of the cuff is important in order to obtain an accurate reading; too large, and the patient’s blood vessels will not be sufficiently occluded to obtain anything that could be considered a true blood pressure and if it is too small, it may make the patient uncomfortable/cause injury or fail to stay in situ once fully inflated.
- Measure the blood pressure on both of the patient’s arms. The arm with the highest measured reading should be used for the blood pressure measurement proper.
- Take multiple readings from the same arm, and document the average
Manual Blood Pressure Measurement

Performed with a cuff inflated and deflated by the practitioner.
Place the cuff onto the patient’s arm and palates the brachial artery. Once a pulse can be felt, inflate the cuff until the pulse disappears, noting the reading on the pressure gauge. This figure is the estimated systolic pressure.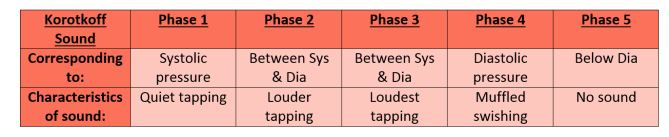
Place the diaphragm of the stethoscope over the brachial artery and inflate the cuff to 30mmHg above the estimated systolic pressure. Deflate at a rate of 2-3mm/sec until phase 1 of the Korotkoff sounds is heard. This is the systolic pressure.
Continue to deflate the cuff until the sounds disappear. The last Korotkoff sound heard is the diastolic pressure
Automatic blood pressure measurement
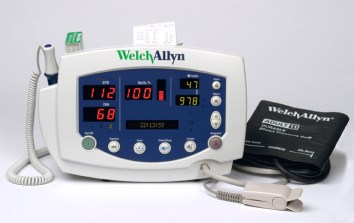
The practitioner attaches the cuff and operates the measurement unit, which inflates and deflates the cuff without any further input.
Auto-monitors can be set to inflate to a present pressure, or set to increase the pressure until a reading is gained.
Factors affecting blood pressure measurement
- Smoking, alcohol and caffeine have been shown to raise blood pressure, so it is recommended that the patient refrain from these for at least 30 minutes prior to measurement
- A full bladder can raise blood pressure 10-15mmHg
- talking, blood pressure could rise 10-15mmHg
- Emotional states can affect readings. Stress and White Coat Hypertension can elevate measurements
- Inadequate rest prior to testing can raise BP by 10-20mmHg
- Temperature, particularly a cold environment will raise pressure readings.
- Positioning of the patient:
- Crossed legs can cause a 2-8mmHg increase
- Unsupported arms: can increase/decrease 2mmHg every inch the arm is above/below the heart
- unsupported back can cause a 6mmHg increase
- A cuff placed over clothing can impact systolic pressure by 10-50mmHg
Ref:
Handler, Joel. The Importance of Accurate Blood Pressure Measurement. The Permanente Journal (2009) 13:3: 51-54
Long, JM., J.J. Lynch, N.M Machiran, SA Thomas, KL Manilow. The effect of status on blood pressure during verbal communication. Behavior Science (2004) 5:2: 165-172.
O’Brien E, R. Asmar, L Beilin, Y Imai, J. Mallion, G. Mancia, T. Mengden, M. Myers, P. Padfield, P. Palatini, G. Parati, T. Pickering, J. Redon, J. Staessen, G. Stergiou, P. Verdecchia. European Society of Hypertension recommendations for conventional, ambulatory, and home blood pressure measurements. Jounral of Hypertension (2003) 21: 821-848.
Pickering, T.G., J.E. Hall, L.J. Appel, B.E. Falkner, J. Graves, M.N. Hill, D.W. Jones, T. Kurtz, S.G Sheps, E. J. Roccella. Recommendations for Blood Pressure Measurement in Humans and Experimental Animals: Part 1: Blood Pressure Measurement in Humans: A Statement for Professionals From the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Hypertension (2005) 45:142-161.
http://www.faqs.org/nutrition/Hea-Irr/Hypertension.html
http://www.infobloodpressure.com/factors-affecting-BP-readings.html